New mRNA therapy aims to restore missing enzyme in Gaucher: Study
It offers potentially more effective alternative to enzyme replacement therapy
Written by |
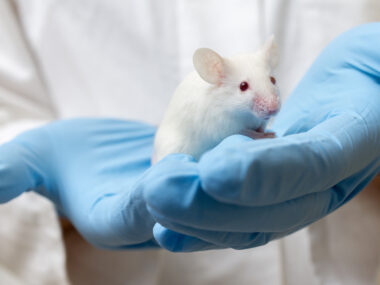
Researchers have developed a therapy using messenger RNA (mRNA) that has the potential to restore production of the enzyme missing in people with Gaucher disease, according to a mouse study. Messenger RNA is the template molecule that carries genetic instructions for protein production.
The therapy, packaged in tiny fatty particles, boosted enzyme activity in cells and in the livers and spleens of mice. These organs are commonly affected in Gaucher disease.
Since an mRNA therapy directs the patient’s own cells to produce the missing enzyme, it offers a potentially more effective alternative to current enzyme replacement therapy (ERT) for Gaucher.
According to researchers, the “mRNA approach as a protein replacement therapy may represent the transformative power of biomedical innovation, potentially setting a new standard for genetic disorder treatments.”
The study, “Development and optimization of human glucocerebrosidase-encoding mRNA for Gaucher disease therapy,” was published in Biochemical and Biophysical Research Communications.
Existing therapies limited by high cost, side effects
Gaucher disease is a rare genetic condition marked by a deficiency of glucocerebrosidase (GCase), an enzyme that degrades the fatty molecule glucocerebroside (Gb1) within cellular compartments called lysosomes, which serve as the cell’s recycling centers.
Without this enzyme, Gb1 builds up inside lysosomes, particularly in immune cells called macrophages that engulf large amounts of molecular waste. This creates enlarged “Gaucher cells” that primarily accumulate in the spleen, liver, and bone marrow, leading to disease symptoms.
The two main treatment options for Gaucher are ERT and substrate reduction therapy (SRT). ERT is designed to deliver a functional version of the GCase enzyme to help cells clear excess Gb1, while SRT works to reduce Gb1 production in the first place.
While these therapies effectively reduce Gb1 and alleviate symptoms, they are limited by high cost, frequent dosing, and side effects. Moreover, lab-made GCase cannot cross into the brain and spinal cord, limiting its benefit for Gaucher patients with neurological impairments.
mRNA therapy would instruct patient’s cells to produce missing enzyme
Scientists in China are exploring a new approach to treating Gaucher using mRNA, a naturally occurring molecule that acts as a template for protein production.
Rather than delivering GCase from outside the body, as in ERT, an mRNA therapy would instruct the patient’s own cells to produce the missing enzyme. In addition, mRNA therapy can be designed to include signals that direct GCase production to lysosomes, whereas delivery of external GCase to lysosomes can be inefficient.
To explore this approach, researchers began by designing and testing different versions of mRNA molecules encoding GCase. After screening multiple combinations, one candidate was stable and produced more than six times the GCase enzyme activity of the lowest-performing version.
In cells lacking GCase to mimic Gaucher, lysosomes became enlarged due to Gb1 accumulation. But when the team treated these cells with the mRNA therapy, GCase activity was restored, and lysosomal size was reduced. Delivery to cells via lipid nanoparticles (LNPs), spherical sacs composed of fatty molecules, further boosted GCase production and activity.
The implications of mRNA technology extend beyond the [Gaucher disease] community, paving the way for developing similar therapies for a spectrum of genetic diseases.
To test whether the mRNA therapy works in a living organism, the researchers administered the mRNA packaged in LNPs directly into the bloodstream of mice. In one group, a fluorescent marker was fused to GCase to allow visual confirmation of where the protein was being produced. GCase was detected in the liver at both six and 12 hours after injection.
In a follow-up experiment, mice received 1.5 mg/kg of mRNA-LNP and were assessed at six, 12, 24, 36, and 72 hours post-injection. GCase protein and enzyme activity were detected in both the liver and the spleen at all time points assessed.
The team also tested whether the mRNA triggered an immune response by measuring anti-GCase antibody levels in blood. No significant difference in antibody levels was observed between mice that received the mRNA-LNP and those that received a saline control, indicating no notable immune activation in the first two days following administration.
“This study focuses on applying GCase-encoding mRNA for treating [Gaucher disease] as a potential alternative therapy to overcome the limitations of current treatments, such as ERT and SRT,” the researchers concluded. “The implications of mRNA technology extend beyond the [Gaucher disease] community, paving the way for developing similar therapies for a spectrum of genetic diseases.”